CAR T-cell Therapy for Childhood Cancers

What is CAR T-cell therapy?
CAR T-cell immunotherapy, developed in recent years, is emerging as a new treatment option, particularly for rare and aggressive childhood cancers. The method is mainly used for patients who do not respond to conventional treatments or whose disease has relapsed. Instead of relying only on external drugs, this approach focuses on using the patient’s own immune system to fight cancer. According to the National Cancer Institute, CAR T therapy works by modifying a patient’s immune cells so they can better recognize and attack cancer cells.

How does the treatment work?
The treatment process starts by collecting T cells from the patient’s immune system. These cells are then genetically engineered in a laboratory to recognize specific proteins found on cancer cells. After this modification, the cells are multiplied and infused back into the patient’s body, where they begin targeting cancer cells directly. Research published in Nature Reviews Clinical Oncology shows that CAR T-cell therapy involves genetically engineered T cells that can specifically recognize and destroy cancer cells, representing a personalized approach to treatment.
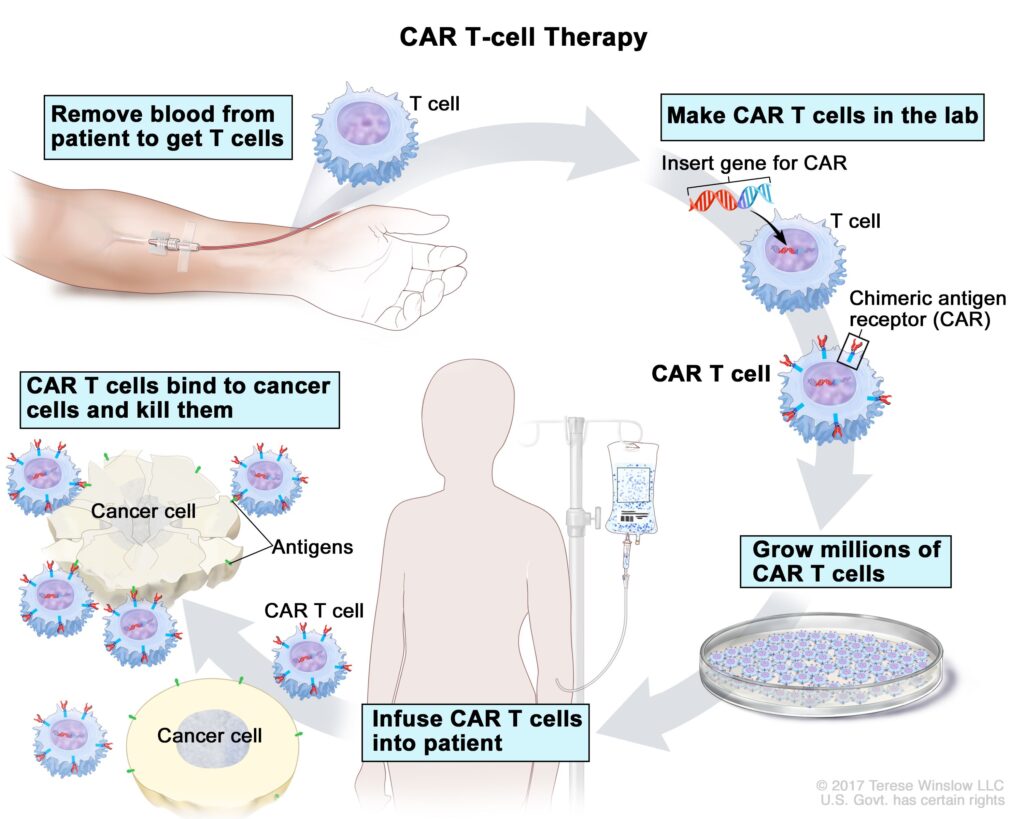
A targeted alternative to traditional treatments
Experts highlight that CAR T-cell therapy differs from chemotherapy and radiotherapy by being more targeted. While traditional treatments can also harm healthy cells, this method directs the immune system specifically toward cancer cells. This targeted mechanism is considered especially relevant in cases where cancer does not respond to standard treatments, offering a different therapeutic pathway supported by recent clinical findings.
Clinical results in pediatric patients
Clinical studies indicate that CAR T-cell therapy has shown significant results, particularly in children diagnosed with acute lymphoblastic leukemia. According to research published in The New England Journal of Medicine, some patients who did not benefit from previous treatments achieved long-term remission after receiving CAR T therapy. These findings position the therapy as a viable option in cases with limited alternatives.

Risks and side effects
Despite its potential, the treatment requires careful monitoring due to possible side effects. One of the most serious complications is cytokine release syndrome, which occurs when the immune system becomes overactive. According to findings in Blood Journal, this condition may lead to symptoms such as high fever, low blood pressure, and organ dysfunction, making close medical supervision essential.

Cost and accessibility challenges
CAR T-cell immunotherapy is also associated with high costs and complex production processes, as it is developed individually for each patient. This limits its availability, since not all healthcare centers have the necessary infrastructure to provide this treatment. According to the American Society of Clinical Oncology, financial and logistical challenges remain key barriers to the wider use of CAR T therapies.

Ongoing research and future applications
Researchers continue to explore how CAR T technology can be adapted for other types of cancer. Current studies focus on expanding its use beyond blood cancers, particularly toward solid tumors. Institutions such as the World Health Organization also emphasize the importance of innovative treatments in improving global cancer outcomes, highlighting the role of continued research in this field.
